COVID Deaths in People Under the Age of 25 highlight Fatal Year
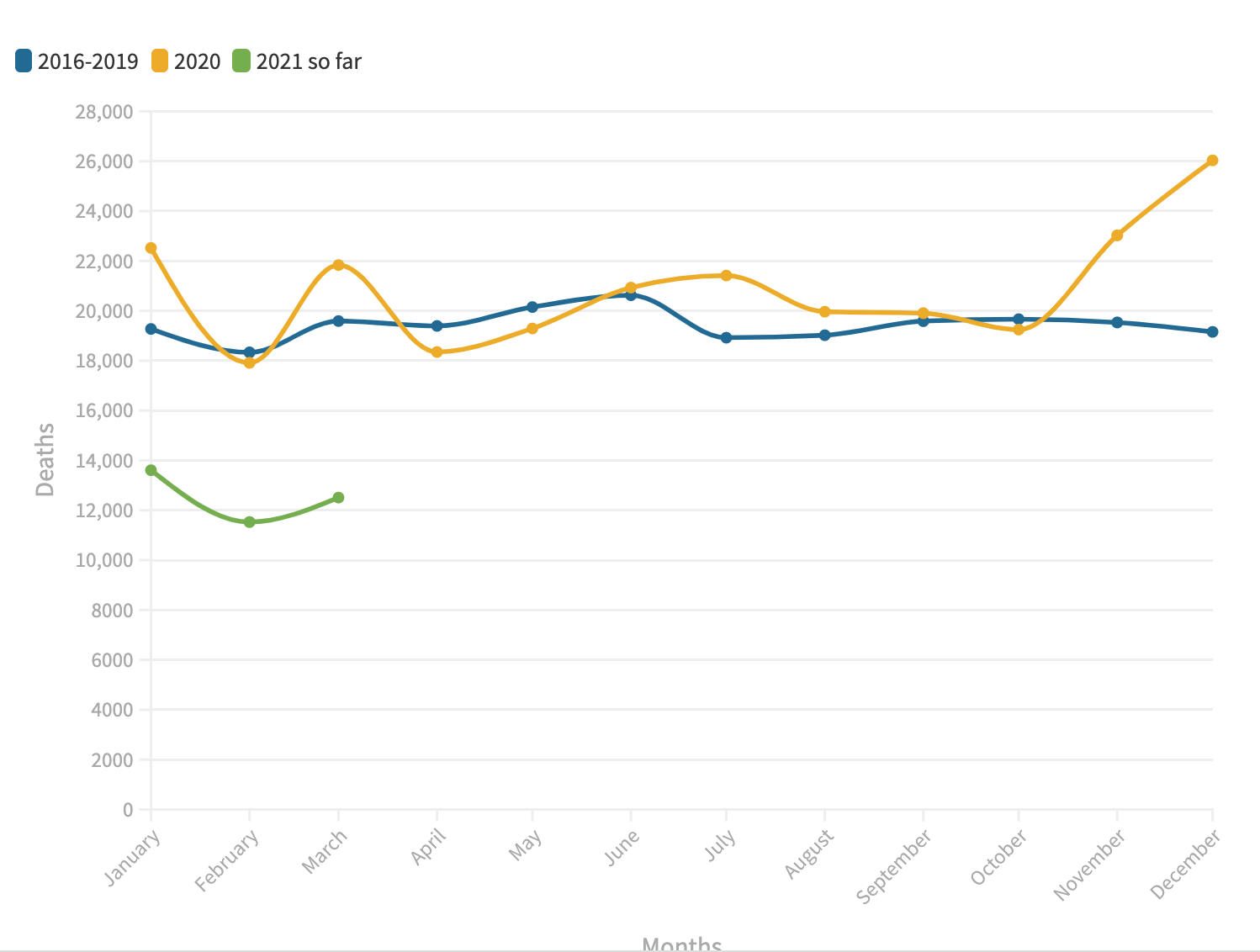
The ongoing COVID-19 pandemic has affected more age groups more severely than others. To date there have been 557,486 deaths resulting from the coronavirus. Data from the CDC shows that the bulk of deaths were people over the age of 50. It is well established that COVID-19 has a greater effect on the elderly than it does on the young. However, this is not to say that younger people are immune from the virus and death. 2020 saw an 8.7% increase in deaths from 2019 in people under the age of 25. 2020 also saw a 3.5% rise in deaths of people under the age of 25 when compared to the yearly average between 2016-2019.
While the numbers for 2020 are not significantly greater than the numbers in any other year measured. 2020 unlike the other years shown has a significant public health event that drives its numbers up. COVID-19 has proven to not be overly deadly to this age demographic. Collectively in 2020 and 2021 there have been 8,485 COVID Deaths for people under the age of 25.
But as it concerns excess death reporting there was an increase in deaths since the onset of the pandemic. Combined death data from the years 2020 and 2021 subtracted from COVID deaths in this age demographic left 11,483 deaths over the average.
In an interview with Nature Medicine, Professor Kevin McConway suggests that looking at excess deaths is the best way to understand COVID’s effect on mortality. “Just looking at the numbers of deaths attributed to Covid-19 is problematic. What counts as a Covid-19 death is defined differently in different countries.”
Inconsistencies in the way that COVID deaths are reported have been well documented. Anesthesiologist from Maryland, Dr. Nikolus Visnich describes a chaotic scene on the frontlines of the pandemic, “We were unprepared, undermanned, lacking in PPE, and no one knew what the policies were.” “Everchanging policies and procedures made it harder to compartimentalize what was occurring,”” Dr. Visnich explained.
What Dr. Visnich did not describe was a significant uptick in the hospitalizations of people under the age of 25. Dr. Visnich explained that elective procedures had to be halted and that the hospital was noticeably emptied of anything that wasn’t related to COVID. Dr. Visnich did experience a rush of appendectomies in teenagers at one point during the summer. Dr. Visnich suggested that less people were coming to hospitals. He thought this was two-pronged, there was a significant public health crisis and there wasn’t time to focus on other things, but he also suggested that people fear hospitals in the current climate. “If people can’t feel safe in a space designed to help them, then they won’t seek help.”
Not relying on public services in times of need no doubt shifted the public’s attitude towards the medical system. Attitudinal shifts result in behavioral changes. Changes that very likely caused an increase in death. To understand what an increase in death means is to understand what is happening in the big picture of society. Discrepancies in the way COVID deaths are reported from place to place coupled different societal actions in response to a pandemic are what must be sorted to understand the implications of excess death in 2020.
McConway in the same interview suggests that the pandemic’s wide-reaching effect can drive up deaths in certain directions while driving them down in others. To McConway it is a matter of defining what a COVID death constitutes. “That entirely avoids the issue of what counts as a COVID death, and it also picks up extra deaths that occur because of changes to health services that restrict access to cancer treatments, for example, as well as possible reductions in deaths, maybe because there’s less traffic and fewer road accidents during lockdowns.”
Policies differ from hospital to hospital and state by state. The states with the highest populations such as California, Florida, New York, and Texas reported the most COVID deaths in people under the age of 25.
What we see is that most states didn’t have a death in this age demographic, while the major population centers such as Texas, California, Florida, and New York all experienced death tolls in the hundreds. The majority of states did not have a COVID death in the under 25 age demographic, but the major increases in California, Florida, New York, and Texas have accounted for a rise nationwide.
The data that excludes COVID deaths shows a similar trend to the COVID death data. The major population centers Texas, California, Florida, and New York lead the way in excess deaths in people under the age of 25.
Spikes in excess deaths have accompanied spikes in COVID deaths in this age demographic. The size and population of states that demonstrate this trend should be noted. Even in normal years, California, Florida, New York, and Texas are among states with the highest deaths in those under the age of 25.
It may be years before we fully understand where the 11,000 excess deaths have come from since the start of the COVID-19 pandemic. The effects of the pandemic have had major societal ramifications. Homicides were up 35.2% from 2019 in 2020. Non-COVID hospitalizations were low. True lasting impacts are yet to be seen.
2020 was a chaotic year, lockdowns, societal unrest, and economic struggles were present. To what extent these factors had on the youth of the country is yet to be determined. But what the numbers show is an above average year in the death of young people resulting from the effects of an ongoing pandemic.
To fully understand the ramifications of COVID-19, death reporting ought to be better categorized and defined. The lack of a consistent definition of what a COVID death is, no doubt has muddled the picture on where the uptick of death has come from. But it is clear where COVID goes death follows.